Thirteen-year-old Jahi McMath is dead. That’s the conclusion of Paul Fisher, the chief of Pediatric Neurology at Stanford University, who was appointed by an Alameda Superior Court judge to examine the girl and make the final determination about whether this Oakland eighth-grader is alive or dead. He concluded that the child lying in the hospital bed at Children’s Hospital in Oakland is in fact dead, with no hope of recovery.
He said she had an irreversible brain injury and shows complete absence of cerebral function, meeting all criteria for brain death, listed by professional societies and the state of California.
Alas, that conclusion hasn’t satisfied Jahi’s grieving family, whose painful, tragic denial, fueled by what they call a strong religious faith, has been exploited and amplified by an attorney with questionable ethics, groups with a political right-to-life agenda, and media members who seem enamored with the made-for-TV-medical-drama suspense aspects of this storyline.
If there is anything positive that can be gained from this situation is that it is prompting good discussions in responsible media outlets and in private homes about end-of-life issues. And perhaps it is encouraging people to consider carefully at how they would want to die, or how they would make decisions in regards to a loved one who is terminally ill or who has suffered a traumatic brain injury and can only stay alive through mechanical means.
Maybe the best place to look for answers to these questions are doctors and health professionals themselves. Find out what life-saving measures they would choose — or rather, not choose — for themselves. You would be very surprised.
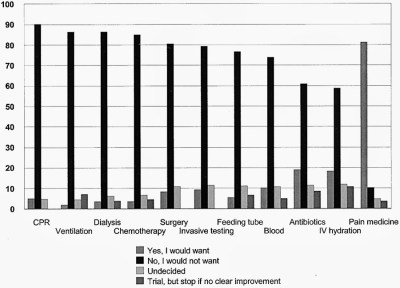
“The Bitter End,” is a January 2013 segment on the PBS radio show RadioLab that looks at a decades-long Johns Hopkins University study on doctors, including asking doctors about their own views on medical care and dying.
The study shows (see chart above) that up to 90 percent of doctors, surveyed for a hypothetical scenario in which they suffered irreversible brain injury, would decline mechanical ventilation, CPR and dialysis. Up to 80 percent would say “no” to a feeding tube. Of course, they know things we lay people don’t know, including what it really means to get CPR (only about 8 percent of people survive, and the rest are in pretty horrible shape) and what it means to be kept alive by a breathing machine.
“What it buys is misery we would not inflict on a terrorist.”
This quote comes from Ken Murray, a doctor was interviewed for the RadioLab report and who has written several articles about how doctors think much differently about death than patients.
The misery he refers to involves patients getting cut open, perforated with tubes, assaulted with drugs, and hooked up to machines — specifically to mechanical ventilators — in what doctors know is a “futile” attempt at care.
“All of this occurs in the intensive care unit at a cost of tens of thousands of dollars a day. What is buys is a misery we would not inflict on a terrorist,” he writes in an article “How Doctors Die: It’s Not Like the Rest of Us, But It Should Be.”
He more specifically addresses the agony of mechanical ventilation in the RadioLab interview. To use mechanical ventilation, doctors need to paralyze the patient, so she can’t move, though she might still be fully aware of what’s happening around her, Murray said. Mechanical ventilators usually involve inserting an endotracheal tube into the windpipe. This can be profoundly uncomfortable, as sometimes, other reports say, the machine doesn’t quite sync up to the patient’s natural rhythm for breathing.
When my father was on a mechanical ventilator for a few days after heart surgery in 2002, the doctors strongly suggested he be heavily sedated so that he wouldn’t be mostly unconscious until it was removed. My father eventually came off the ventilator, and lived for another eight months, but had trouble swallowing and later developed pneumonia and other infections. Watching my father on the ventilator convinced me that I never want to be on one.
In a blog post for the Center for Health and Media Policy at Hunter College, RN Mauricio Berrio Orozco asks whether prolonged mechanical ventilation causes needless suffering, especially in patients surviving a devastating brain injury. “Many of them are conscious, but a good prognosis is basically impossible. They do not have even the slightest chance of recovering their previous level of functioning.”
Orozco also points out the serious problems that can arise from long-term ventilation. These patients are at serious risk for infections and ventilator-associated pneumonia, huge pressure ulcers and muscle atrophy from inactivity.
Murray adds that some of the treatments we offer to critically ill patients are often “worse than the disease. You may be prolonging life but not for very long. The life you have left is misery.”
So, if Jahi is still alive, as her family and their supporters insist, then keeping her indefinitely hooked up to a mechanical ventilator carries the risk of condemning her to days and months of agony. If she is alive, it sounds like she’ll need to be paralyzed, heavily sedated and constantly monitored for infections, ulcers and muscle atrophy.
The family has received support from a brain-injury treatment center dedicated to Terri Shiavo, the Florida woman whose case in the mid-2000s sparked a fierce nationwide end-of-life debate, according to the Contra Costa Times. The organization, run by a former hairdresser, revealed earlier this week that it was helping Jahi’s family get her transferred to a facility in New Jersey, that claims to be “about preserving life and treating brain-injured patients with care and dignity.”
The mechanically ventilated reality of Jahi’s death–or life, as her family asserts–seems a far cry from dignity. If she’s alive, then it could be misery, as Murray describes. The medical interventions necessary could lead to profound suffering. Did the Terri Shiavo organization, or the facility accepting her transfer, explained those facts to her family?
But if she’s dead, as all the experts say, the only misery and suffering would be to her dignity. It’s time for her family, already coping with profound grief, to accept that she’s gone.